Implementation Toolkits: Resources
1. Outcomes table
2. A table of challenges
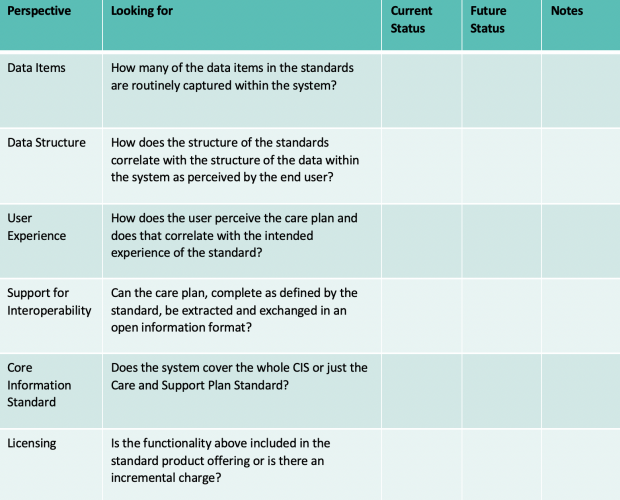
3. System supplier diagnostic table
4. Designing your own stocktake
5. The key elements from Change Laboratories for conducting a successful stocktake
6. CHAT – A vehicle for inter-personal dialogue
7. Stakeholder drivers
8. Start with the end in mind
9. Examples of a convoy approach (PCSP specific)
10. Stakeholder grid
11. Benefits Evaluation Grid
12. Features of a good stocktake
13. Simulation workshops
14. Further resources
2. A table of challenges
3. System supplier diagnostic table
Download printable version by clicking here: System Supplier Diagnostic.doc
4. Designing your own stocktake
The matrix will help guide how you design the workshop and how you organise the outputs. The matrix is designed to prompt you to align with:
• The dimensions of change (Policy, Practice, Culture, and Technology)
• The types of intelligence you are seeking (Current practice, Desired future practice, Plans for implementation, Real/perceived barriers, Enablers, Motivations for change and enhancement, What success will look like).
Download printable version by clicking here: Conducting workshops matrix
5. The key elements from Change Laboratories for conducting a successful stocktake are:
• Successive rounds of discussion move the conversation forward rather than starting at the beginning every time you work with the group or fresh groups.
• Adopting the use of ’stimulus material’ or ‘mirror data’ – using objects, documents, videos, or relevant testimony to get a conversation started and refining the stimulus material for each successive round of conversation so it incorporates what has already been contributed. To maintain the focus on PCSP standard implementation we used clinical scenarios and care plans as the stimulus.
• Leaning into the discomfort of disagreement and tension to actively find new ways of doing things – particularly relevant when working with multi stakeholder/multi professional cohorts.
• Maintaining focus on the shared objective of all the ‘activity systems’ (in this case stakeholder or professional groups) on the shared objective of improving care through the adoption of the PCSP standard.
6. CHAT - A vehicle for inter-personal dialogue
1. Who are the subjects of learning, how are they defined and located?
2. Why do they learn, what makes them make the effort?
3. What do they learn, what are the contents and outcomes of learning?
4. How do they learn, what are the key actions or processes of learning?
7. Stakeholder Drivers
“As an early implementer of the new standard I want to work with the NHS E/I funded project so that I can accelerate and enrich my immediate and future adoption of the standard for the benefit of patients. I anticipate that in order to meet the standard, I may have to make changes in clinical and operational practice and initiate technical changes (delivered either by my team or my software supplier(s)). I want to be able to plot the route map, understanding the changes I need to make, when to make them and the best sequence in which to implement them to maximise the benefits for my patients.”
“As a patient or service user I want to receive joined up care to avoid repeating information which can be traumatic for me and to know that the care professionals providing my care are working to the current standard and with the best joined up information so that my care is safe, efficient and empowering to me.”
As a care system also adopting (or planning to adopt) the standard, I want to draw from a set of materials so that I benefit from prior learning to avoid known pitfalls / nugatory work whilst also leveraging from materials so that I can produce the relevant business cases and transformation plans / route maps efficiently.”
“As the system vendor (technology partner) I want to understand what the current standards are and how those standards are applied/used so that I can ensure my technology supports the best practices based on the open standard.”
“As NHS E/I I want to support (fund) and deepen the adoption of the standard firstly with the two Early Implementers and then with the further 10 identified care systems so that I am assured that the benefits of the standard are realised for the care systems and their populations.”
“As the PRSB I want to show how the adoption of the standards benefit care and maintain a knowledge base of materials for future adoption of the standard by Integrated Care Systems and their suppliers.”
8. Start with the end in mind
How to roll out pilot projects widely
Click to read more
Experience shows that there is often a drop in energy - “voltage drop” - at the point when successful pilot projects expect to roll out to other relevant parts of the system. One way of minimising this is to think about spread, adoption, and sustainability, and how these will be phased, from the outset, for example identifying which areas are well-placed to emulate the pilot sites quickly – “fast followers”- and which may need more time and support before they are ready for the proposed change.
A Stocktake will be particularly useful to identify viable trailblazer, pilot, and adoption sites.
Click to read more
Stocktake will be particularly useful to identify viable trailblazer, pilot, and adoption sites. The best approach entails identifying a small number of people from these "fast follower" areas who are engaged with the pilots, can shape the work, be well informed, and are aware of the challenges of adoption in their own areas. So that these can influence the programme throughout its course.This change process is iterative and rarely a simple linear progression.
9. Examples of a convoy approach and how it was applied to the implementation of PCSP standard
One version of this convoy might have three “vehicles”/ workstreams:
-
1.
Implementation of a system of Personalised care and support planning for patients in relation to their severe mental illness (SMI) needs. -
2.
Connecting with others across the system so that these plans become one component of a holistic PCSP covering all needs. -
3.
Enabling the digital sharing of these plans so that they can be accessed wherever and whenever they are needed by all those authorised to do so.
An example of a likely constraint might be the time taken to procure or to upgrade digital systems with the capability to support personalised care and support PCSP) planning in full. Work on the design of documentation and of the systems of care that underpin the new approach can be undertaken while technical specifications and procurement are in hand, and will be valuable to refine your technical specification.
10. Stakeholder Grid
Hover over headings to learn more about their meaning.

When noting each type of stakeholder, this is a useful place to also think about their RACI characteristics…
- What responsibilities do they have? What are you relying on them to achieve PRSB standard implementation.
- For what and to whom are they accountable? How will their decision-making or judgment impact the success of your PRSB standard implementation?
- Do you need to consult with them? How and why? Do they have insights, experience, specialist knowledge, or skills that will contribute to successful PRSB standard implementation? How much weight is attached to their views and in what specific areas (e.g. user perspective regarding person-centredness, technical know-how to influence system design, clinical experience to influence changes in practice, etc)
- Do they need to be kept informed and if so how? Is this a matter of routine formal or informal reporting, and is it generic briefing or tailored?
12. What are the features of a good a stocktake?
-
Provide a vehicle for telling people about your transformation objective and give them a chance to get on board with the ideas.
-
Enable you to check your understanding of the ‘problem’ you might be trying to fix and to better appreciate how your sense of the situation is different from the view other stakeholders might have based on their different knowledge and experience, for example as point-of-care professionals.
-
Offer an opportunity to bring representatives from different stakeholder and professional groups together to collectively reflect on what they have in common, how they are different in their approaches, culture, and language, and how they can work towards a shared objective.
-
Be designed to reflect that the implementation of the PRSB Standards is a people-based cultural endeavour and cannot succeed without the hearts, minds and professional expertise of all your stakeholders.
14. Further Resources
The following links are provided to direct you to a wealth of additional support and guidance relevant to:
- National policy,
- PRSB and Personalised Care and Support Planning/Plans,
- Business processes and transformational change,
- Engagement and people development
Title/Description | Why it’s included | Where to find it (URL or link to folder) |
|---|---|---|
National Policy links | ||
NHS Mental Health Implementation Plan 2019/20 – 2023/24 NHS Policy document | Background to the prevailing policy context | https://www.longtermplan.nhs.uk/wp-content/uploads/2019/07/nhs-mental-health-implementation-plan-2019-20-2023-24.pdf |
NHS Long Term Plan NHS Long term Plan website | Background to the prevailing policy context | https://www.longtermplan.nhs.uk/ |
Clinically-led review of NHS access standards NHS website sets the scene for the clinical review of standards and makes recommendations for the introduction of new waiting time standards for mental health (and other areas) | Background to the prevailing practice environment in the NHS | https://www.england.nhs.uk/clinically-led-review-nhs-access-standards/ |
Community Framework | community-mental-health-framework-for-adults-and-older-adults.pdf (england.nhs.uk) | |
PRSB, PCSP standard and care planning | ||
PCSP Conformance Pack | The PRSB assess conformance using self-assessment by the supplier who provides evidence of the way the standard works. This is then reviewed and assessed by a team of expert assessors and validated by a PRSB expert. The expert will also run test cases through the supplier’s system to provide direct evidence in a sandbox environment.
If you would like a copy of the conformance pack, please use the second link to submit a request to the help desk. | |
Why do we need standards for health and care record | The NHS and social care are some of the most information-rich organisations on the planet, but health and social care are behind the way most of us live our lives online with instant access to information at the press of a button. The NHS is working to enable all IT systems across the health and care sector to talk to each other, called interoperability, which will ensure that the right information is available when it is needed to support safe, reliable care. | |
The PRSB Personalised Care and Support Plan Standard | Personalised care planning standards will also help to enable people to manage their own care, with the support of a wide range of services including GPs, hospitals, occupational therapy and social care. The standard will help citizens and health and care professionals to get the right information when they need it, in order to personalise care, and improve the experience for the patient, their carer and their families. | |
Writing good care plans A PDF guide to writing good care plans from Oxleas NHS Foundation Trust | This booklet is for anyone who wants to understand how to plan care and would like to develop skills in care planning. This includes people who use health and social care services and their families and carers, those who work in health and social services, and those who work in partner organisations. | http://oxleas.nhs.uk/site-media/cms-downloads/Writing_Good_Care_Plans_Oxleas.pdf |
Implementation of Dialog and Dialog+ Video introduction to Dialog and Dialog+, and PROM used in ELFT | Through service user and carer testimony this video introduces the main principles underpinning Dialog and Dialog+ | https://dialog.elft.nhs.uk/Home/A-Video-Explaining-Dialog |
Introduction to ReQoL Video introduction to ReQoL, a PROM used in SYB | Through service user, care professionals and research testimony this video introduces how ReQoL was developed and how it’s used | https://www.reqol.org.uk/p/overview.html |
About me Video introduction to ‘about me’ in care planning. | A carer talks about how they have been using digital technology to share information with health and care professionals to improve the quality and cohesion of a service user’s care. | |
Comprehensive Model of Personalised Care | This video which is an animation clarifying the personalised care and support model from NHS England | |
Delivering universal personalised care AN NHS website about personalised care | This link to the NHS England site on Universal personalised care. It includes the lead contact points for Personalised Care Demonstrator Sites which were established in 2019/20 (ironically one of which is SYB) but also links to lots of other reinvent guidance. | https://www.england.nhs.uk/personalisedcare/upc/ |
Personalised Care case studies An NHS website hosting general case studies related to personalised care | This link to a series of case studies showing the benefits of the implementation of elements of the Comprehensive Model for Personalised Care; these examples are from all dimensions of health, not specifically mental health | https://www.england.nhs.uk/personalisedcare/upc/comprehensive-model/case-studies/ |
Joined–up care: Sam’s story A video from the King’s Fund about why joined-up care is important for service users and the NHS | The jargon of ‘integrated care’ is much-used in health policy and management circles. But why does ‘integrated care’ matter? And what will it mean for patients? This short animation aims to bring integrated care to life for anyone involved in improving patient care. If those working towards integrated care can share this vision with others in their local health and care system, then there is a real chance they can make integrated care happen. | |
Business process and transformation links | ||
Quality Improvement resources form ELFT ELFT QI website as a gateway to useful resources about quality improvement | East London NHS Foundation Trust (ELFT) is a provider of mental health and community services, to a population of approximately 1.5 million people, mainly across East London, Bedfordshire and Luton. They define Quality improvement as (QI) going beyond traditional management, target setting and policy making. QI methodology is best applied when tackling complex adaptive problems – where the problem isn’t completely understood and where the answer isn’t known – for example, how to reduce frequency of violence on inpatient mental health wards. QI utilises the subject matter expertise of people closest to the issue – staff and service users – to identify potential solutions and test them. | |
Information governance | The legal framework governing the use of personal confidential data in health care is complex. It includes the NHS Act 2006, the Health and Social Care Act 2012, the Data Protection Act, and the Human Rights Act. This site offers advice and guidance on appropriate information governance in your context. | https://www.england.nhs.uk/ig/about/ |